New Zealand’s demand for mental health services is skyrocketing. The 2018 mental health inquiry acknowledged the magnitude of the issue and the barriers to wellbeing for those suffering from addiction and a wide range of mental health disorders, promising much-needed change and improvements to the national system, including accessibility and staffing issues.
Despite the promise, frontline mental health workers like psychiatrists are overwhelmed, waiting lists are still months long, and people are turning up at emergency rooms at a critical point. Had access to mental health care been available earlier, it could have provided interventions to help those afflicted manage their mental health challenges and prevent them getting to this point.
With 78% of New Zealanders being either personally affected by mental distress or are close to someone who is, and the current referral pathway for mental health services struggling to support those in need, many mental health workers in private practice are now proactively stepping up to bridge the gap. They are working with those facing mental health issues before the problems progress and the patients reach breaking point. There’s just one big accessibility barrier for those seeking treatment in private practice: the upfront cost.
With appointment fees necessary to keep private practices operating, clinics across New Zealand have now taken matters into their own hands to care for new patients without the burden of the full upfront cost. Here’s how they’re doing it, how you can access a mental health provider without the full funds sitting in your bank account, and why doing so is more important now than ever.
Long Waiting Times For Mental Health Services Are Having Dire Consequences
Mental health is an extremely broad topic encompassing a range of conditions. As a quick snapshot of the status of common mental health conditions conclude that:
- One in five New Zealand adults suffer from a mood or anxiety disorder, according to the recent National Health Survey
- One in five kiwi kids will be affected by depression by 18 years old
- Almost one in five will meet the criteria for an anxiety disorder by 19 years old
- 685 people are suspected to have died by suicide during 2019. While this is not the highest rate in the world, we do have one of the highest youth suicide rates in the OECD
- 151,000 18-24 year olds report drinking hazardously
- 103,000 kiwis are estimated to struggle with an eating disorder, with 10% of those with eating disorders estimated to die within 10 years and 26% of people with eating disorders attempting suicide
- 70% of people with eating disorders in New Zealand do not have access to the help they need
When it comes to addressing and managing these and many more mental health issues across all age groups, the longer it takes to receive help, the more difficult recovery can be – both to mentally work through it, and in light of the physical symptoms that may be associated. This is one of the reasons why accessing help early is linked to better health outcomes – before the effects either start to, or add further disruption to a person’s job security and income, schooling, personal and family relationships and other aspects of their physical health.
Unfortunately under the public system, access to public services are only taking longer for all. Despite the strong focus and cash investment into the sector, waiting times for children and teenagers trying to access mental health care has increased by almost two weeks since 2017. Wellington has produced reports of waiting times that exceed six months for children and teenagers with severe mental health needs.
Privately, the cost of accessing timely mental health services is a major deferring factor, with up to 39% of New Zealand adults being reported to delay seeing their GP when they have a genuine medical concern, indicating similarly poor statistics for accessing mental health specialists or seeking referrals from their GP.
Mental Health Challenges In A Changing World
Equally as important as having access to the right care for existing or longstanding mental health issues, is being able to rapidly access help for new problems as they arise as a result of changing circumstances. One example is New Zealand’s lockdown restrictions. From the first lockdown in 2020, 80% of those surveyed said they experienced feelings of anxiety and loneliness, with a 40% increase in the call volumes to the mental health helpline through April 2020 alone.
Pregnancy is another example of a temporary yet important stage. A first-of-its-kind NZ study looking at over 6,000 pregnant women found that 12 percent experienced symptoms of depression. As untreated depression is linked to postpartum depression, preterm delivery and low birthweight babies, there should be no delay in accessing mental health services if they are needed.
HealthNow: The Preferred Solution For Private Clinics
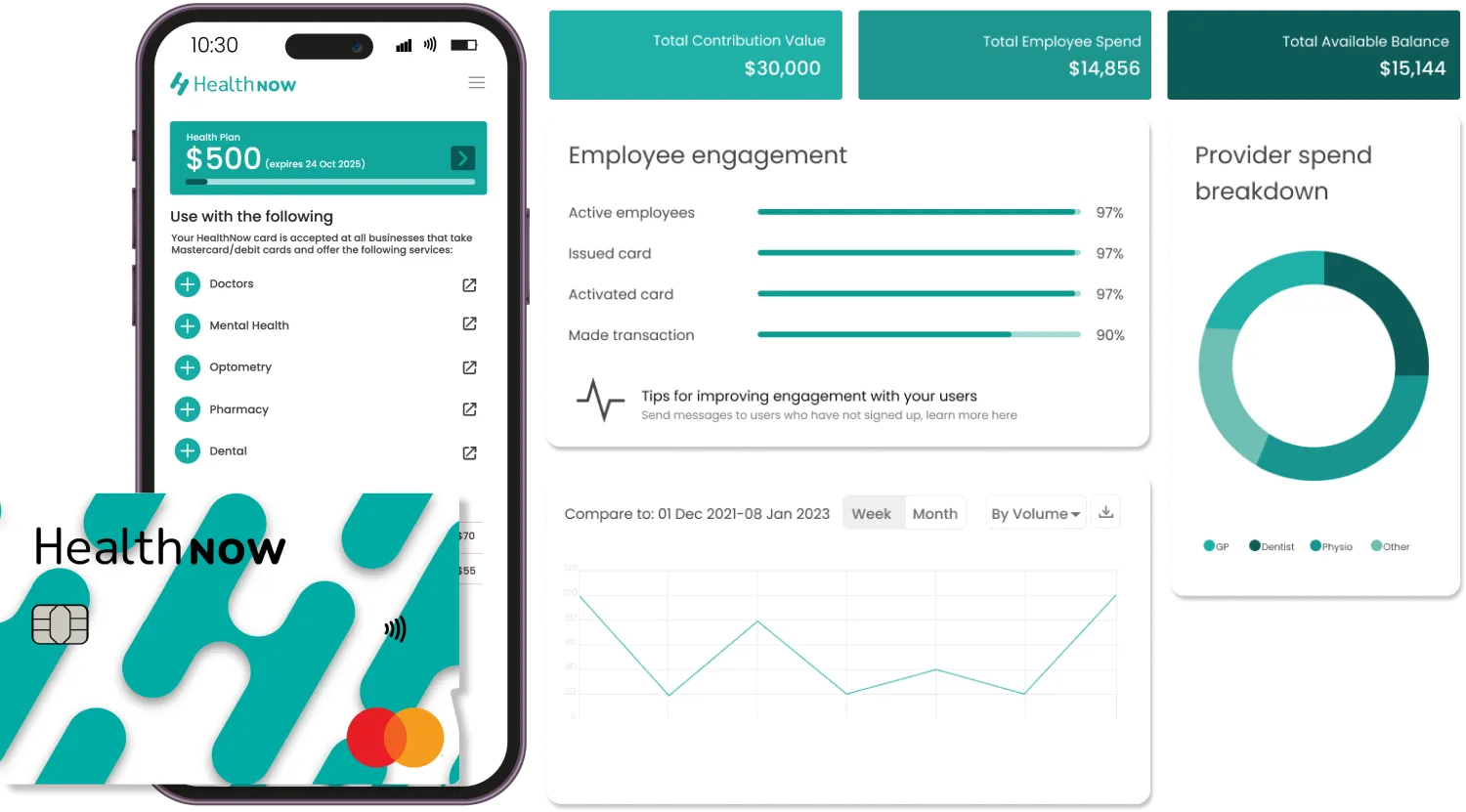
With national improvements to mental health accessibility, waiting times and staffing feeling like a long waiting game at the expense of the health and wellbeing of New Zealanders, mental health specialists and private clinics across the country are now taking matters into their own hands by partnering with HealthNow, New Zealand’s first Buy Now Pay Later (BNPL) service for healthcare.
HealthNow’s goal is to make healthcare more accessible to anyone that needs it, the moment they need it without delay, and without further financially disadvantaging those trying to take control of their mental health by not charging consumers any fees or interest. Instead of paying the full upfront costs, appointment fees are split into multiple smaller payments over a maximum of six weeks.
Using this service, psychiatrists, psychologists, mental health counsellors and other health professionals are now seeing patients in need the same week that they book in to call – with last minute cancellations enabling some to get an appointment on the very same day.
To start using HealthNow and getting the care you need without delay, Sign up on our app and use it easily when it comes time to pay for your appointment. You can also check out HealthNow’s full benefits and features , including a health wallet to store funds set aside for health services that can be contributed to by others including your employer.